Podiatry Billing – General Medicare Coverage Guidelines
By: Cal LaGroue
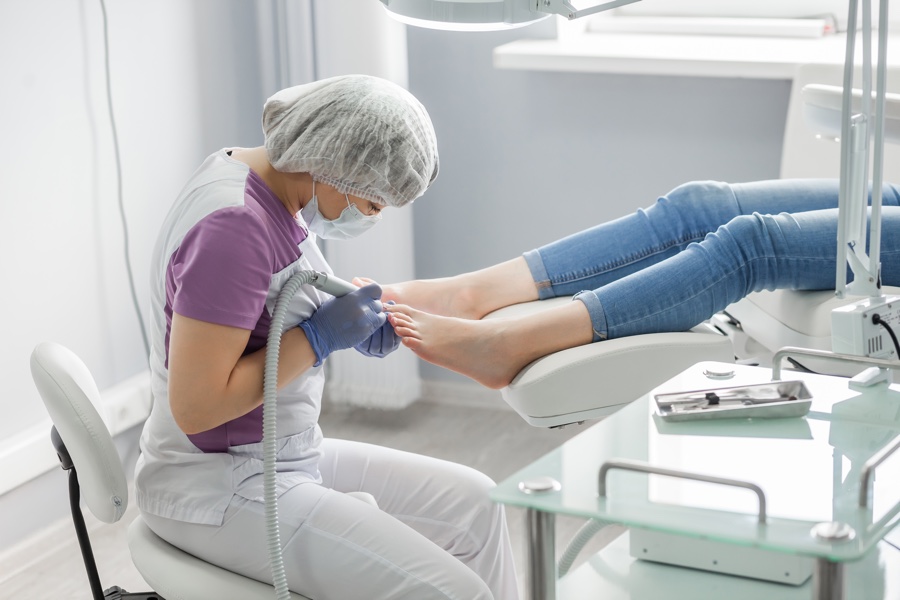
In this article, we’ll discuss various common disorders within the field of podiatry, But more importantly, we’ll discuss when Medicare covers professional treatment for these disorders. A large percentage of foot care is classified as routine, and thus not covered by insurance. The reasoning being that ‘routine care’ does not require the skills of a medical professional. So, in order to avoid podiatry billing nightmares, it’s important for providers and patients to know the distinguishing factors that define eligibility for podiatry Medicare coverage.
Home Health Billing Requirements: An Overview of Medicare’s Eligibility Standards
By: Gilbert Johnston
To Qualify for Home Health Care Under Medicare, Three Requirements must be Met:
The patient must be:
1) confined to his/her home
2) in need of skilled services, AND
3) be under the care of a physician & recommended for home health care by a physician
This article explains, in detail, what actions Medicare considers sufficient to meet each of these three requirements. This is a useful guide for both patients and clinicians looking to develop a firm understanding of the insurance coverage requirements for home health billing.
Surgery Billing – A Guide to Medicare’s Global Surgery Package
By: Robbin Grayson
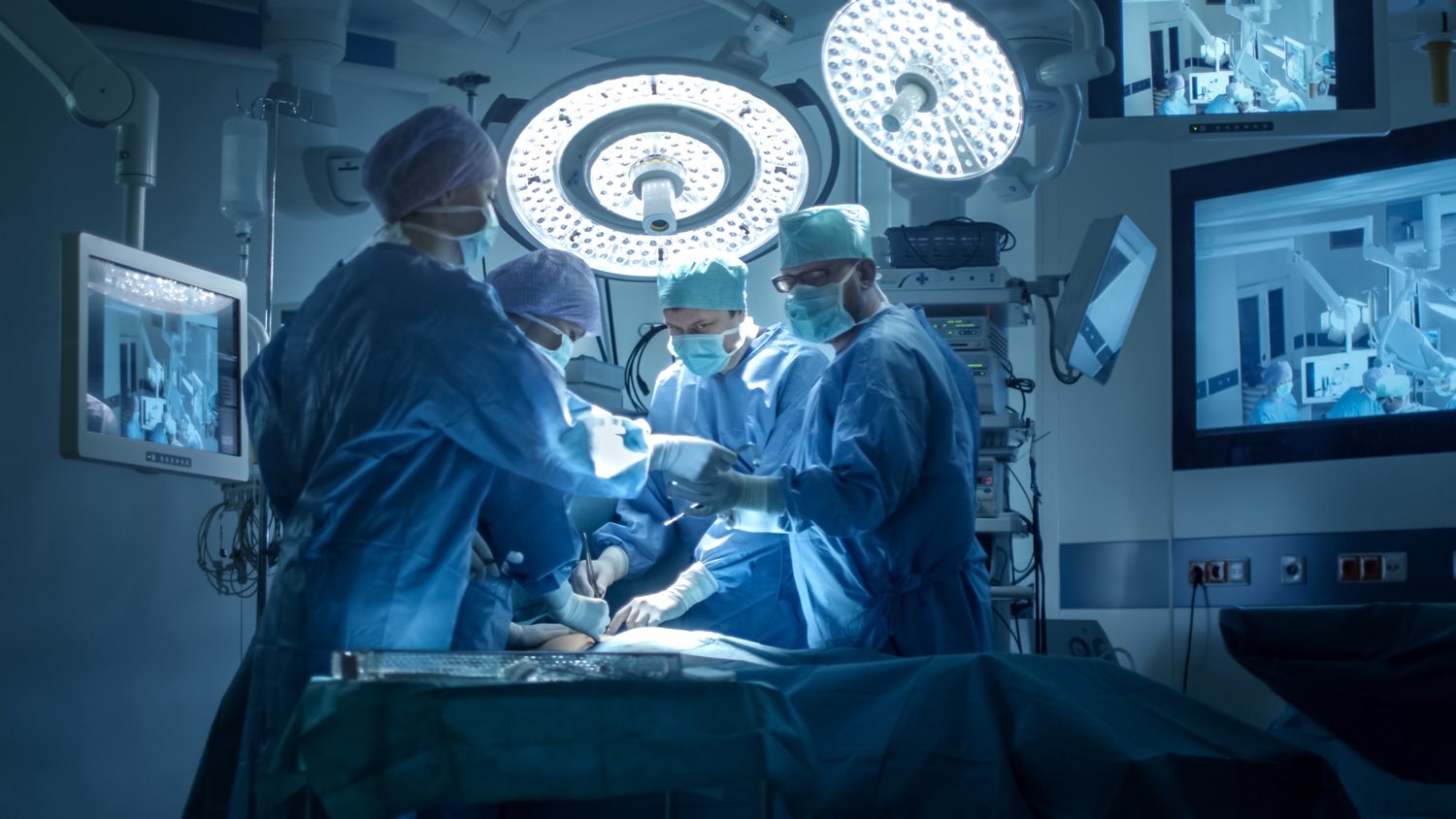
When it comes to medical billing for surgery, there are various claim submission requirements within Medicare. The largest and most broadly applied is called The Global Surgery Package, or more simply, Global Surgery.
Global surgery refers to all the necessary services performed by a surgeon before, during, and after a surgical procedure. It also includes any necessary services performed by members of that surgeon’s team (provided they practice within the same specialty).
Telemedicine Guide: Medicare Coverage and The Medical Billing Process
By: Gilbert Johnston

Every year, telemedicine grows in popularity. More than half of U.S. hospitals already have some sort of telemedicine program, and countless more hospitals are currently developing programs. By 2022, analysts believe that the telemedicine industry will be worth as much as $70 billion.
To accommodate this growing healthcare trend, commercial health insurers are increasingly adopting new telemedicine coverage plans, as well as expanding existing plans. For physicians looking to grow their practices, now is the time to jump into Telehealth, as coverage has expanded to the point where it makes fiscal sense. In fact, most mid-range insurance plans now cover telemedicine to some extent.
However, before jumping into this new form of care, it’s important to understand how the reimbursement process works. As with most new forms of medical treatment, The Centers for Medicare and Medicaid Services (CMS) has set the initial coverage standards through Medicare. The commercial carriers have followed suit, with similar coverage rules.