Medical Billing Rates – What Prices to Expect for Specific Billing Services
By: Robbin Grayson
The most common question medical billing companies hear is:
“What are your prices?”

It’s a perfectly reasonable question. Price is a major factor in any business decision. Plus, medical billing company prices aren’t exactly readily available. And when rates are listed, the’re often vague or misleading.
In this article, we’ll attempt to clear up some of the confusion surrounding medical billing service rates. We’ll also give you an idea of what specific services to expect for a given price, along with the factors that go into determining that price.
Wondering what price you should expect for the specific billing services you need?
Check out our RCM Price Calculator
Background: What has lead to the current billing industry market and prices?
Medical billing companies have existed for decades, but in the past 10 years or so, the industry’s business model has changed dramatically.
This change can be attributed to two main factors:

1) Growth
There’s been a great deal of growth in the medical billing industry in recent years, the cause of which is multifaceted. The simple explanation involves a combination of technological advances and regulation changes; specifically, more complex coding requirements (ICD-10), more intensive privacy regulations (HIPAA, HITECH Act), and increases in the use of Electronic Health Records (EHR) software. As of result of these changes, medical billing has become a more difficult process; thus, increasing the demand amongst clinicians for third party billing experts.
2) Consolidation
Like the healthcare industry in general, the medical billing industry has experienced major consolidation. Small, local billing companies used to make up the vast majority of the market. While they’re still quite common, their market share has declined significantly in the past decade. This decline is largely due to large, publicly-traded EHR software companies entering the billing market. These software companies came into the billing space with hopes of saturating the market. They offered low prices and attempted to automate the revenue cycle work. In that respect, they have largely failed. However, they’ve certainly acquired a portion of the billing market and they’ve left a lasting impact in the form of generally lower prices.
The Effect:
Growth and consolidation have lead to a market that is more competitive, but less defined. For the consumer, there are pros and cons to this new medical billing market. The biggest con, which we’ll get into later, is that clinicians often don’t receive the services they thought they paid for. The biggest advantage has come in the form of lower billing prices. Gone are the days of medical billing companies regularly charging 10% or more. Today’s competitive market has forced billing companies of all sizes to lower their prices significantly.
Where do current medical billing prices stand?
The Simple Answer: These days, you’ll see advertising pricing anywhere from 3% to 8%.
The Real Answer: The modern medical billing market is still forming. Norms are still being set. After major price shifts, prices have just begun to settle in the past few years.
Medical Billing Prices: The Reasons Behind the Wide Range
Medical billing prices are typically based upon two key factors:
1) The Attributes of the Client
One factor that will drastically affect the price quotes providers see is: practice characteristics
The fact is, some clients are more difficult and time consuming than others, due to the basic defining elements of their practices. Billing companies look for a few different things when determining what they can afford to charge a client. Below is a somewhat simplified list of what billing companies prefer.
Practice size (number of providers)
Provider type (MD/DO over NP/MS/LC/etc.)
Specialties (amount and type)
Number of Office Locations
Claim volume
Per claim dollar amount
Amount of codes
In basic terms, the best client for a billing company is a large practice, with only MDs, working in one specialty, in one state, and conducting a limited amount of high-cost procedures. While no client is easy, a client with these attributes would create the most straightforward, easy-to-manage workload.
The more uniform the work, the easier it is to manage. A multi-state, multi-specialty practice is going to deal with several different insurance payers and far more rules and regulations. Organizing and managing the work is going to take a larger team with more experience, and thus, cost the billing company more money. It’s that simple. And it’s an unfortunate reality for practices that are more difficult to manage.
Some of the factors above weigh more heavily than others, like practice size and number of locations. And the truth is, most practices fall somewhere in the middle. The closer you are to optimal, the lower the rate you can expect. The farther you fall to suboptimal, the higher the rate you can expect. For some solo MDs, it can be difficult to find a rate below 6%.
Certain providers, like solo therapists, often struggle to find a company that will even take them on as a client. The truth is many billing companies simply can’t afford to take on certain clients. For some solo psychologists in need of relatively comprehensive medical billing services, a company may have to charge above 10% just to break even. And unfortunately, many solo therapists can’t afford to pay that much.
2) The Specific Billing Services Provided
The other biggest reason for the 5% range in medical billing prices is the wide variety of services that billing companies offer and clinicians request.
Let’s be clear. The days of big margins for medical billing companies are long over. Even companies charging around 8% aren’t making a killing. Their prices are higher because they’re providing a lot more services (and often higher-quality services) to their clients.
Similarly, companies charging 3% don’t have thinner margins. They simply offer far fewer (and largely inferior) services. So, when you see advertised medical billing prices online in the 3 to 4.5 percent range, remember that there’s a reason those prices are so low.
In the end, hiring a billing company really comes down to what matters most to the client:
- What level of service do you expect?
- How important is accuracy to your revenue cycle? I.e. how costly are denials?
- Do you expect the billing company to handle coding, claims appeals, credentialing, patient collections, data analytics, etc.?
- Beyond billing, do you need help with HIPAA compliance, MIPS, pre-authorizations, etc.?
- Do you care whether your billing team is in the U.S. or oversees? E.g. do you want responsive, articulate customer service?
- Do you need EHR software? Do you want to keep your current software?
These are some of the questions you need to ask yourself. There are a lot of services out there. It’s the provider’s job to figure out both the quantity and quality of services that will benefit them most.
The List of Services to Consider
The modern clinician revenue cycle has several steps:
- Charge Entry
- Claim submission
- Payment posting
- Accounts Receivable
- Claims Appeals
- Patient Statements
- Reporting
On top of those steps, most modern practices also need advice or assistance with other items like:
- Credentialing & Enrollment
- Coding
- Patient Collections
- Patient Inquiries
- Pre-Authorizations
- HIPAA Compliance
- Value-based Care (e.g. The Quality Payment Program, MIPS, & APMs)
- Online Patient Payment Options
- Data Analytics
Plus, there are other factors to consider, like whether offshoring some billing work is acceptable to you. Doing so can help lower costs, but it can also cause major issues when not done correctly and responsibly.
Depending on size and staff levels, a practice may need help with all or only some of the above items.
Average Medical Billing Prices: The Rates to Expect for Specific Services
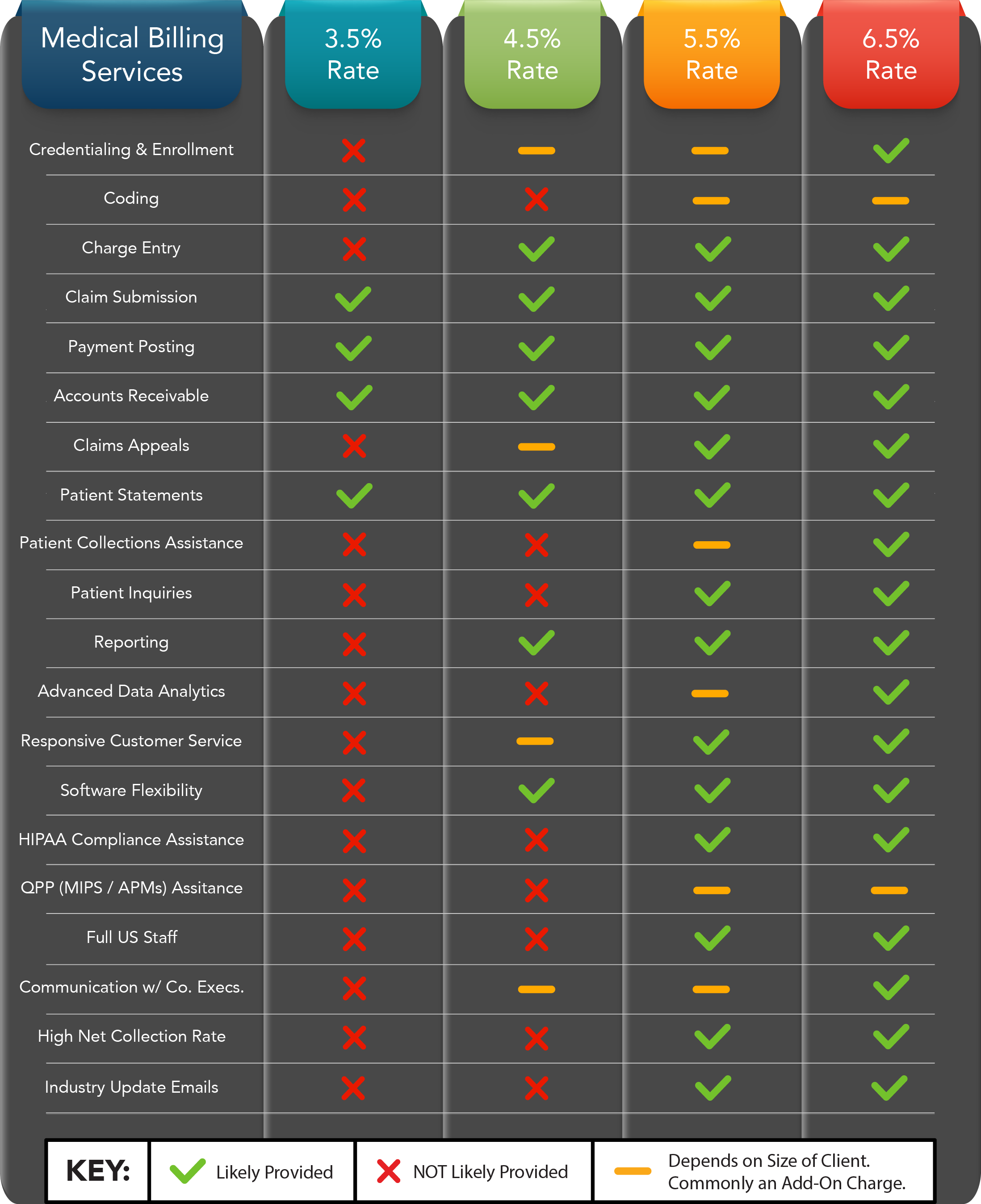
At Valletta, we’ve been providing medical billing services for over 15 years. We study the market closely and consistently. Thus, we have a pretty good idea of what services companies are offering and what prices they’re charging for those services. From our experience, we’ve compiled a chart of the services you should expect at different price points.
This chart is based upon our own experience and market knowledge. It is NOT based on any particular entity. We make no specific assumptions about any individual company.
Chart Breakdown:
Note: The prices listed in the above chart are based on what a relatively “desirable” client may find (see Section 1: “The Attributes of the Client”, above). Less desirable clients may find average rates to be 1-3% higher than the prices listed in the chart.
There are a few different pricing structures in the medical billing industry, but most are percentage-based (i.e. clients are charged based on how much their billing company collects on their behalf). In fact, if pricing is structured on a per-claim basis, you can bet that the services are pretty minimal (i.e. comparable to what you’ll find for a 3% rate).
Again, the different rates come down to the services that are included. For example, some billing companies might charge an average rate of 5.5% for billing. Included in that 5.5% rate are all the general steps of the revenue cycle, from charge entry to patient statements and reporting. Such a company may also offer credentialing, data analytics, patient collections assistance, and MIPS services, but as add-on charges. Requesting some or all of those charges would effectively increase the overall billing rate to somewhere in the 6 to 8% range.
This is the important thing for medical providers to take away from this article. If you’re looking for a particular set of services, you’re going to see similar rates from most billing companies (at least the reputable ones), regardless of what they may advertise. The trick is to find a company you trust, that specializes in and, more importantly, presents themselves as offering the types of services you’re looking for. The fact is, a company that advertises a 3% rate is likely going to excel most at providing the services associated with that 3% rate. A company that talks less about price and more about offering comprehensive, quality services is going to excel at offering more comprehensive, accurate, and responsive billing services (at a rate likely in the 5-8% range).
When you finally pull the trigger and begin negotiating with different billing companies, remember what we discussed earlier. Margins are relatively thin in the medical billing industry. If a price sounds too good to be true, it likely is. So, during negotiations, remember what’s important to you. Are you looking to pay the lowest price possible? Or are you looking to ensure that your financials are optimized in a consistent and reliable manner?
Imagine this. Two companies are offering the same services, but one company is offering a 5% rate while the other is offering 6%. It’s easy to choose the lower price. And maybe that is the right choice. However, it’s more likely that the services of the 5% company will be lesser in the long run. Maybe the staff will be somewhat slower to get back to you. Maybe the amount of denied claims will be a little higher on average. Maybe the company will be less consistent in warning you about payer changes that may affect your reimbursement. But there will likely be a difference. There almost always is. It’s your job to figure out what’s cost effective for your practice. Will that 1% difference in price be more expensive than the cost of slightly inferior work?
Takeaway: Who should you hire? Who should you trust?
The best advice we can give is to take a company’s words to heart. In other words, listen to how medical billing companies advertise themselves.
Again, if a company advertises 3% rates, they likely excel most at providing 3% services. They may also offer more comprehensive services at a higher price point, but their wheelhouse is likely 3%. Would you trust McDonalds to prepare you fresh lobster and caviar? Probably not. It’s the same for bargain-priced billing companies. They operate very differently from higher-priced billing companies. They offshore all of their work and they don’t have the staff in place to handle more complicated revenue cycle tasks. If you hire them for complex billing work, they’ll likely have to outsource various steps to several different companies, which is risky practice at best. So if you want minimal services at a cheap price point, hire the company that talks about low prices. If you want comprehensive, reliable services, hire the company that speaks to that.